Jaw fractures are relatively common injuries in dogs and cats and can have a major impact on an animal’s ability to eat, groom, and live comfortably. The jaw plays a critical role in chewing and holding food, and it also supports the teeth and connects to the skull at the temporomandibular joints (TMJs). Because of these important functions, fractures of the jaw require careful evaluation and repair to restore normal movement, preserve dental health, and prevent long-term complications.
Causes of Jaw Fractures
Trauma is the most common cause of jaw fractures in companion animals. Automobile accidents account for many cases, particularly in outdoor cats. Other causes include falls, bite wounds from other animals, gunshot injuries, and blunt force trauma. In some pets, jaw fractures may occur due to weakened bone caused by advanced periodontal disease. Severe bone loss around the teeth can significantly reduce jaw strength, allowing fractures to occur during normal activities such as chewing.
Types and Locations of Jaw Fractures
Jaw fractures may involve the mandible (lower jaw) or the maxilla (upper jaw), with mandibular fractures occurring more frequently. These fractures often develop near the canine teeth, premolars, or molars, where the bone is relatively thin. Fractures may be classified as simple or complex, depending on the number of fracture lines, and as open or closed based on whether the fracture communicates with the oral cavity. Open fractures are particularly concerning because bacteria from the mouth can contaminate the fracture site.
Fractures may also occur near the temporomandibular joint, which can complicate repair and recovery. Injuries in this region can interfere with jaw movement and increase the risk of joint stiffness or arthritis if not properly addressed.
Techniques Used to Repair Jaw Fractures
Several surgical techniques are used to repair jaw fractures in dogs and cats, and the chosen method depends on the fracture’s location, severity, and stability, as well as the patient’s size and dental condition. One commonly used approach is interdental wiring combined with an intraoral cold cure composite splint. In this technique, orthopedic wire is carefully placed around selected teeth on both sides of the fracture, and ancold cure composite splint is applied to the biting surfaces of the teeth to stabilize the fractured segments. This method requires the presence of adequate, healthy, and stable teeth on both sides of the fracture to support the wire and splint. It is not suitable for animals with significant tooth loss, advanced periodontal disease, or fractures located in areas without sufficient teeth.
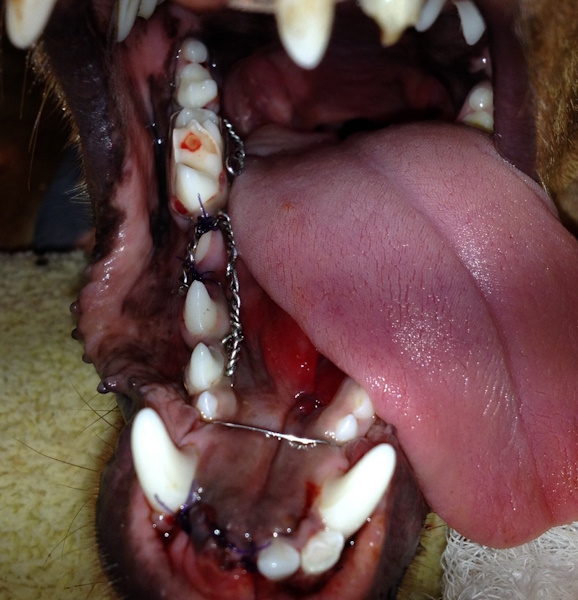
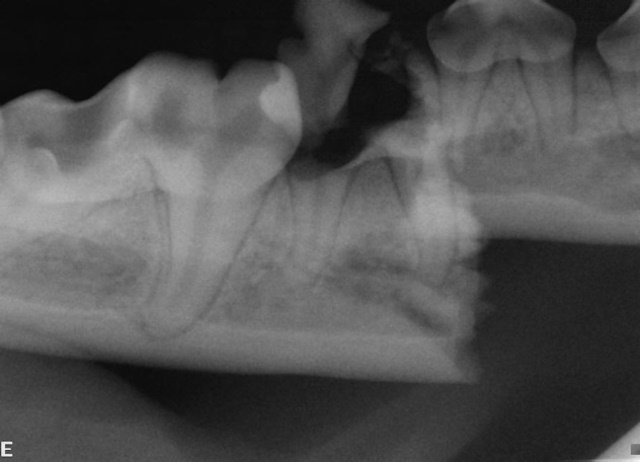
Mandibular fracture is stabilized first with interdental wire and a circumferential wire (image above). Initial intraoral radiograph showing a displaced mandibular body fracture (image below).
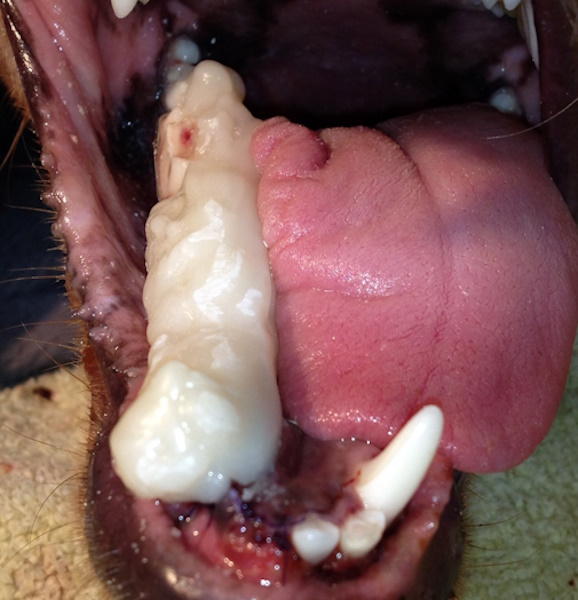
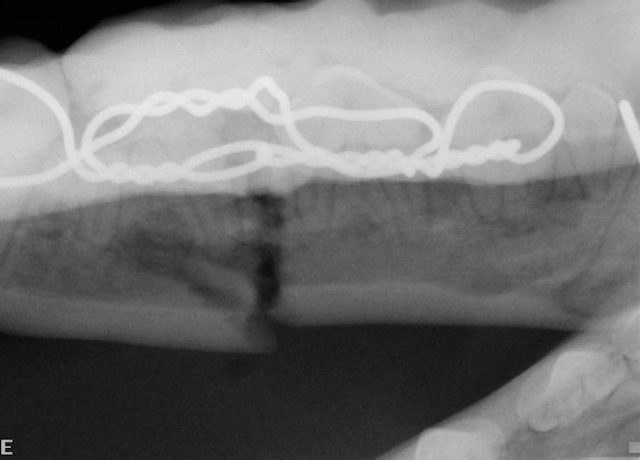
An intraoral cold cure composite splint is placed over the interdental wire to further stabilize the fractured jaw (image above). Intraoral radiograph showing the wire and composite splint. Notice the fracture gap even after careful placement of the wire and composite material (image below).
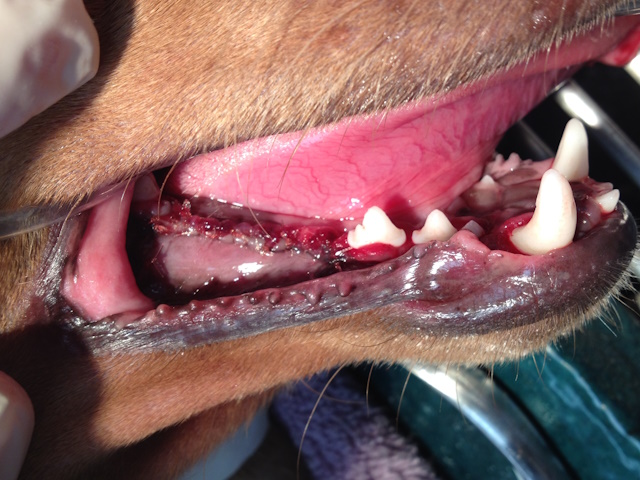
After fracture healing, periodontally and endodontically compromised teeth were removed.
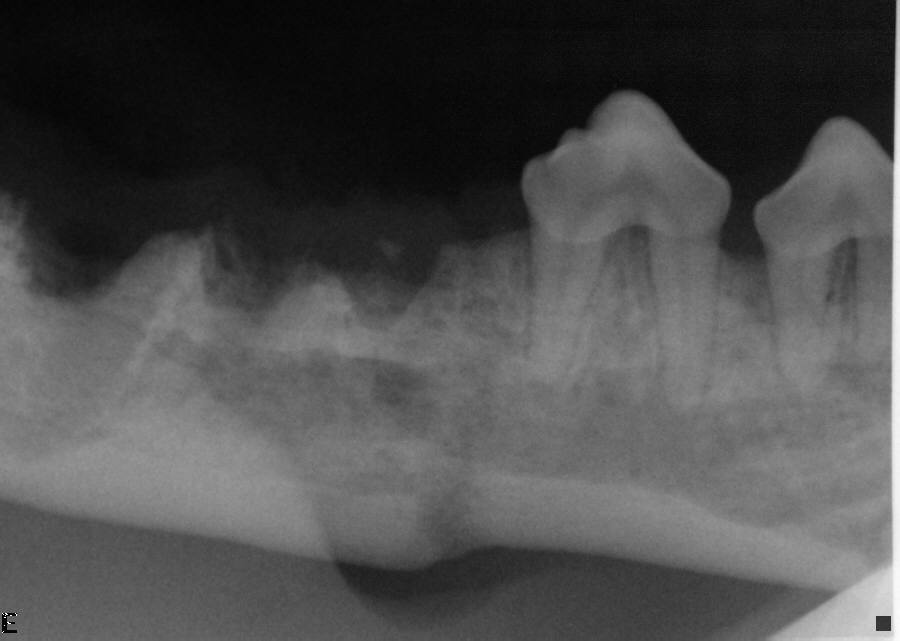
Intraoral radiograph after extractions of endodontically compromised first molar and periodontally compromised fourth premolar teeth. Notice the healed fracture line despite the initial fracture gap.
For more unstable or severe fractures, bone plates and screws may be used to provide rigid fixation. These implants are titanium locking maxillofacial and mandibular mini plates specifically designed for jaw and facial bones. Unlike plates used to repair long bones such as those in the legs, maxillofacial plates are smaller and shaped to fit the thin, delicate bones of the jaw. Locking plate systems allow screws to secure directly into the plate, creating a stable construct while minimizing pressure on the bone and reducing the risk of damage to tooth roots. This method is particularly useful for fractures involving the body of the mandible or maxilla and allows for precise realignment of the jaw.
Other mandibular fracture repair techniques include maxillomandibular fixation using regular and tape muzzles, intraoral cold cure composite splints to bond upper and lower canine teeth, modified labial button technique, and maxillomandibular fixation (MMF) screws and elastic chains (if patient size allows).
A critical component of all jaw fracture repairs is the preservation of normal occlusion. The teeth serve as a guide to align the fractured segments correctly before fixation is completed. Failure to restore proper bite alignment can result in chronic pain, difficulty eating, abnormal tooth wear, and excessive strain on the jaw joints. Careful attention to occlusion during repair helps protect both the teeth and the temporomandibular joints.
Effects on Teeth and Jaw Joints
Jaw fractures often affect the teeth located near the fracture site. Teeth may be loosened, fractured, or infected and may require extraction if they compromise healing. Whenever possible, preserving healthy teeth is important for maintaining jaw stability and function. Fractures involving or near the temporomandibular joint can restrict jaw movement and may lead to joint inflammation or degenerative changes if alignment is not properly restored.
Possible Complications
Complications can vary depending on the repair technique used. Interdental wiring and splints may cause irritation to the gums or damage to teeth if improperly placed or removed. Most interdental wiring and splint treatments induce some degree of periodontal disease around the teeth where these materials are placed. Plates and screws can occasionally loosen or become infected, particularly in open fractures. If strict guidelines are not adhered to, screws may cause tooth root damage. Delayed healing, non-union, or malocclusion may occur if the fracture is unstable or if postoperative care is inadequate.
Postoperative Care
Postoperative management plays a crucial role in successful healing. Dogs and cats are typically placed on a soft or blended diet for several weeks to minimize stress on the jaw. Pain medications and antibiotics are often prescribed, especially for open fractures. Activity restriction is important to prevent re-injury, and follow-up visits allow the veterinarian to monitor bone healing and ensure that normal occlusion is maintained. Owners should watch closely for signs of swelling, pain, or difficulty eating.
Conclusion
Jaw fractures in dogs and cats are serious injuries that require prompt and careful treatment. Successful outcomes depend on selecting the appropriate repair technique, preserving normal occlusion, and providing diligent postoperative care. When properly managed, most pets recover well and regain normal jaw function, allowing them to eat comfortably and maintain good quality of life.
