ORAL TUMORS AND TUMOR SURGERY
Oral tumors are relatively common in dogs and cats and may arise from the mandible, maxilla, palate, tongue, tonsils, or pharynx. Although both benign and malignant tumors occur, the majority of oral neoplasms in small animals are malignant. Tumor behavior is influenced by histologic type, anatomic location, size, and stage at diagnosis, all of which significantly affect treatment options and prognosis.
Diagnosis and Clinical Staging
Definitive diagnosis of oral tumors relies on incisional biopsy, as fine-needle aspiration is frequently non-diagnostic due to inflammation, necrosis, or poor exfoliation of tumor cells. Advanced imaging, particularly computed tomography (CT), is strongly recommended to evaluate tumor extent, bone involvement, and surgical margins. Accurate staging is essential prior to treatment, as oral tumors most commonly metastasize to regional lymph nodes and lungs. Because lymphatic drainage of the oral cavity is variable and unpredictable, sentinel lymph node mapping and biopsy are preferred over routine excision of regional lymph nodes when available.
Treatment
Surgical excision remains the primary treatment modality for most oral tumors in dogs and cats. Complete tumor removal frequently requires mandibulectomy or maxillectomy due to the high incidence of bone invasion. Dogs generally tolerate partial or complete jaw resections well, with rapid return to normal prehension and mastication, whereas cats often experience more postoperative feeding difficulty and commonly benefit from temporary feeding tubeplacement. Adjunctive therapies, including radiation therapy, chemotherapy, and immunotherapy, are selected based on tumor type, grade, and stage.
Prognosis in Dogs
Malignant Melanoma
Malignant melanoma is the most common and biologically aggressive oral tumor in dogs, characterized by early local invasion and a high rate of metastasis to regional lymph nodes and lungs. Surgical excision provides local tumor control; however, long-term survival is significantly improved with adjunctive therapies such as radiation therapy and immunotherapy, including melanoma vaccines. Prognosis is closely associated with tumor size, stage, and mitotic index.
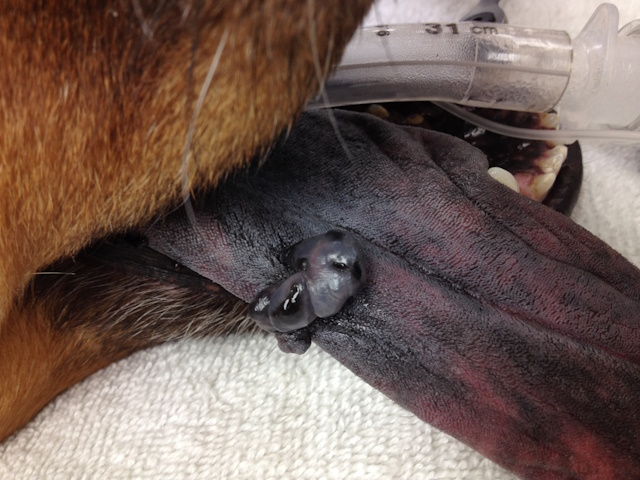
Malignant melanoma on the tongue of a dog.
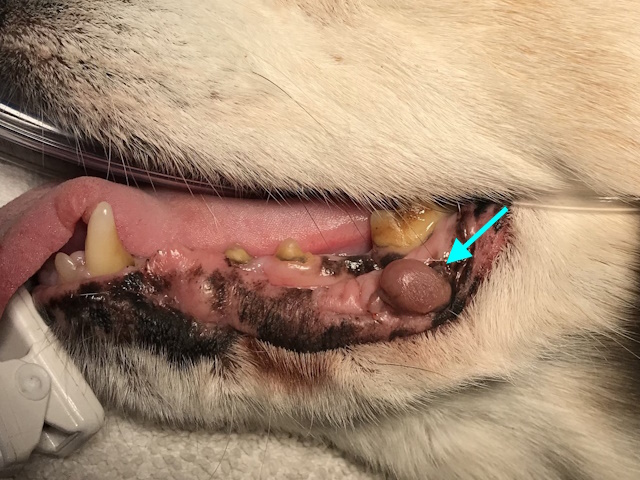
Amelanotic malignant melanoma on the lower lip of a dog.
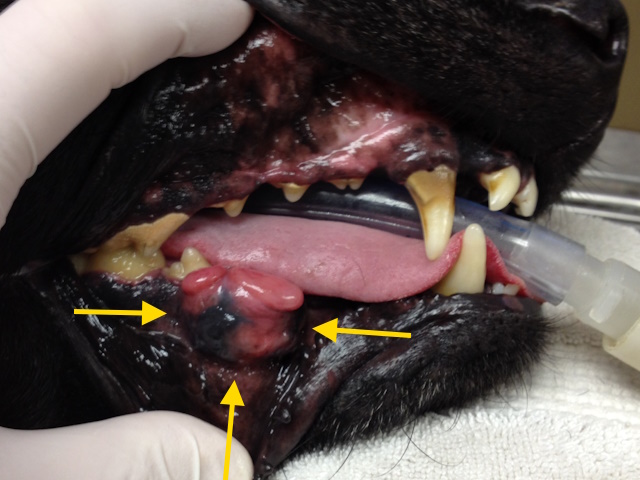
Malignant melanoma affecting the lower jaw of a dog.
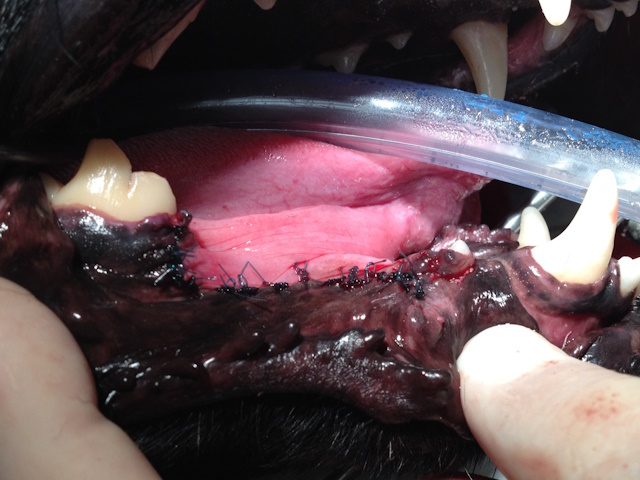
Melanoma was excised using mandibular rim excision.
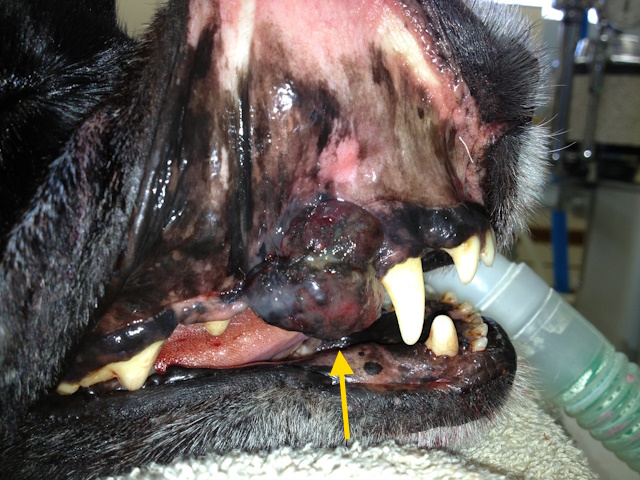
Malignant melanoma affecting upper jaw of a dog.
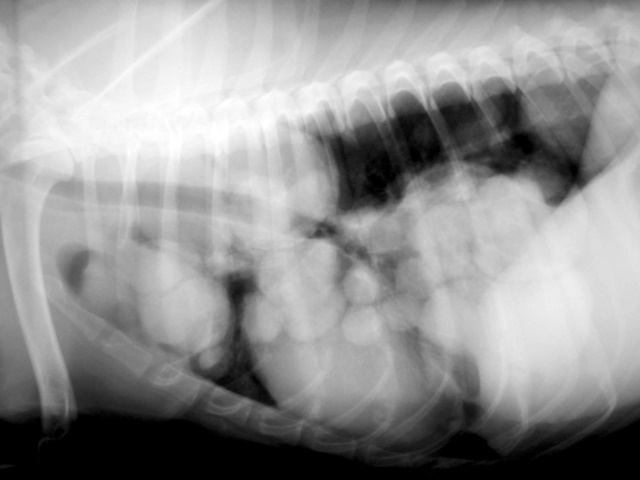
This dog had rapid shallow breathing. Radiographs of the lungs showed diffuse metastatic nodules in the lungs.
Squamous Cell Carcinoma
Oral squamous cell carcinoma (SCC) in dogs is typically locally invasive with a relatively low metastatic rate. Surgical excision via mandibulectomy or maxillectomy often results in excellent local control and long survival times, particularly for early-stage disease. Prognosis worsens with advanced stage, maxillary or caudal tumor location, and high histologic risk scores.
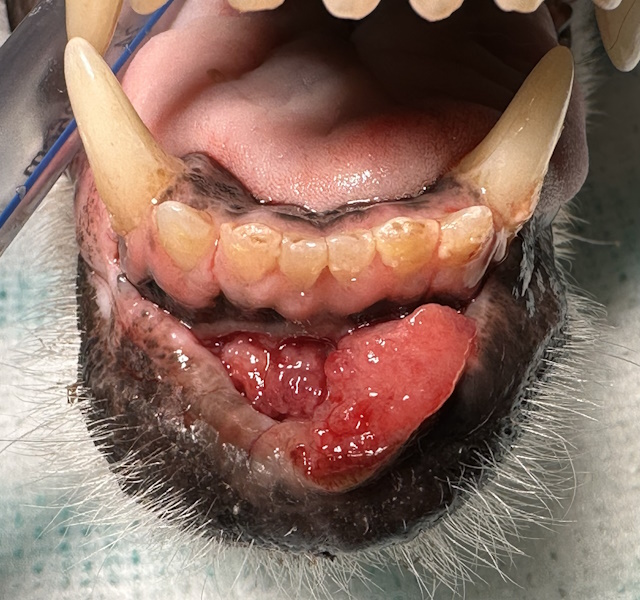
A proliferative, ulcerated and bleeding mass between the lower lips and the lower incisor teeth of a dog.
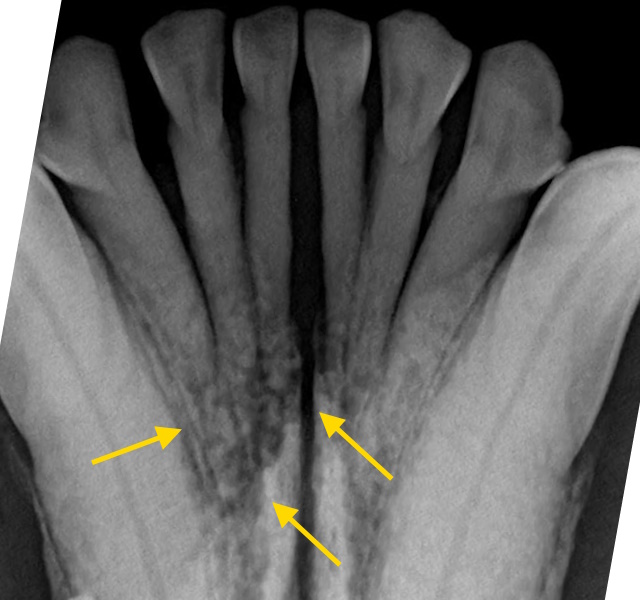
On dental radiographs, mandibular bone destruction was found around the incisor roots.
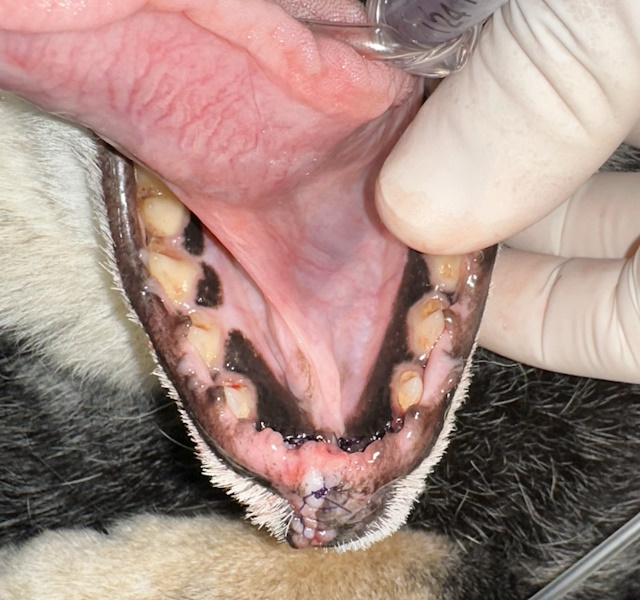
Appearance of this patient’s lower jaw immediately after bilateral rostral mandibulectomy.

The patient’s clinical appearance at recheck 3 monthsafter surgery. Lower jaw is shorter, but this did not affect patient’s eating and quality of life.
Fibrosarcoma
Fibrosarcoma is another locally aggressive tumor with variable metastatic potential; surgery remains the cornerstone of treatment, with radiation therapy considered for incomplete margins or aggressive histologic features.
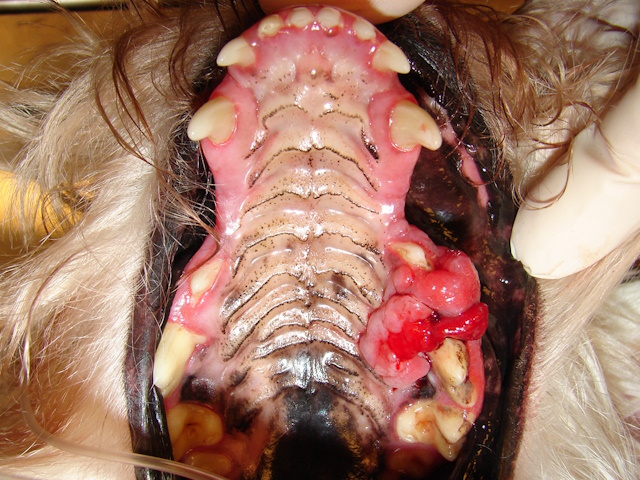
A proliferative and ulcerated maxillary mass in the third and fourth premolar area.
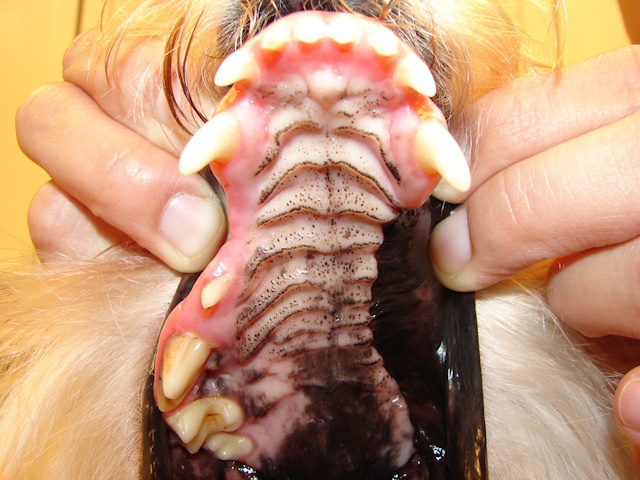
Patient’s doing well at 6 months after surgery with no clinical evidence of recurrence.
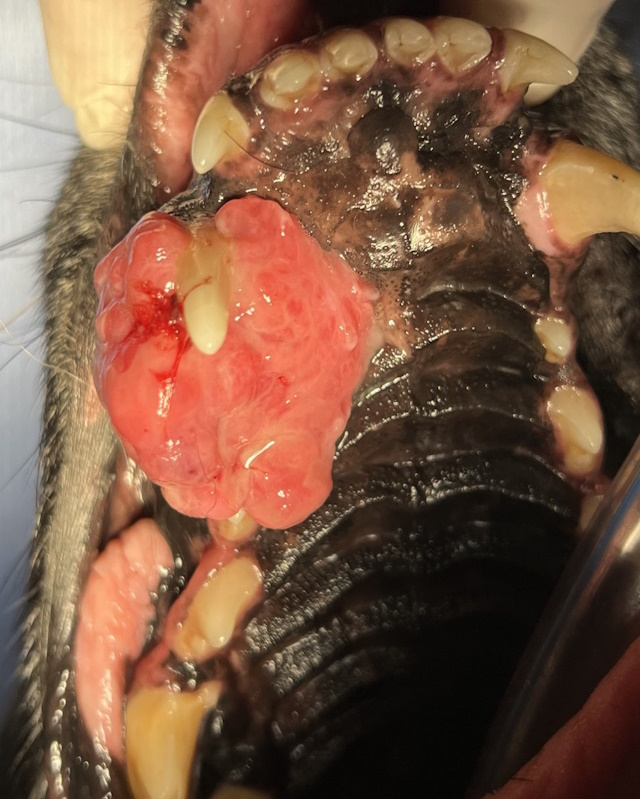
A large, ulcerated mass affecting the upper jaw of this dog.
Recheck after maxillectomy. Surgical site healed well with no evidence of recurrence.
Osteosarcoma
Mandibular osteosarcoma in dogs is biologically less aggressive than appendicular osteosarcoma but still carries a risk of metastasis. Surgical excision combined with adjuvant chemotherapy has been shown to significantly improve survival times compared to surgery alone, with prognosis influenced by histologic grade and proliferative activity.
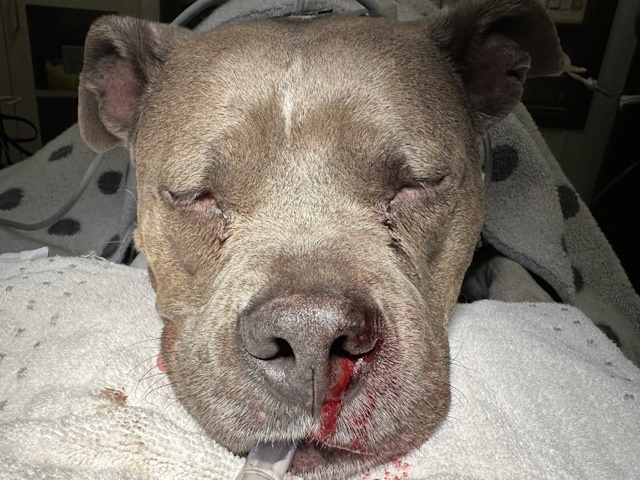
This patient had a history of chronic, intermittent nose bleeds.
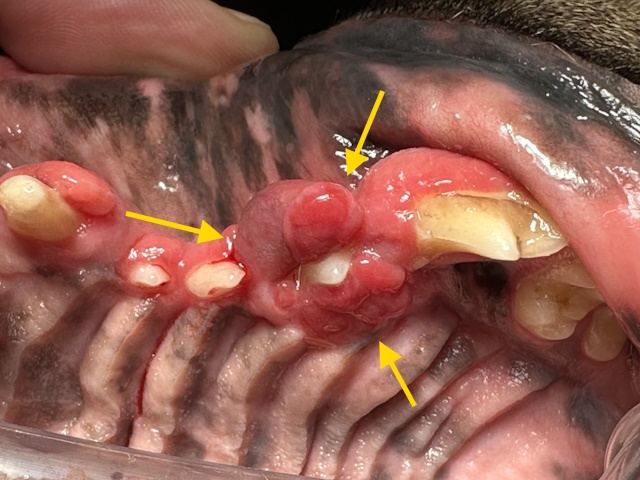
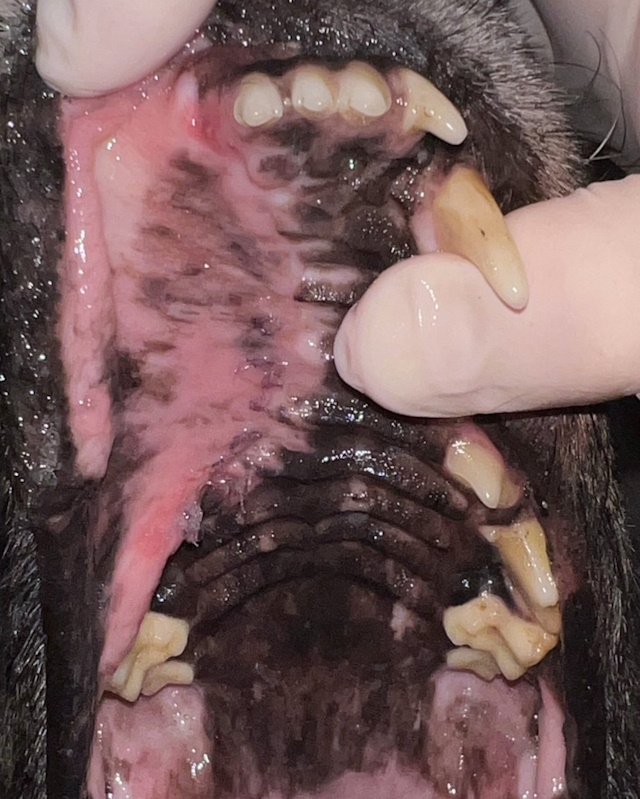
Oral exam revealed a moderate size, ulcerated oral mass around the upper third premolar tooth.
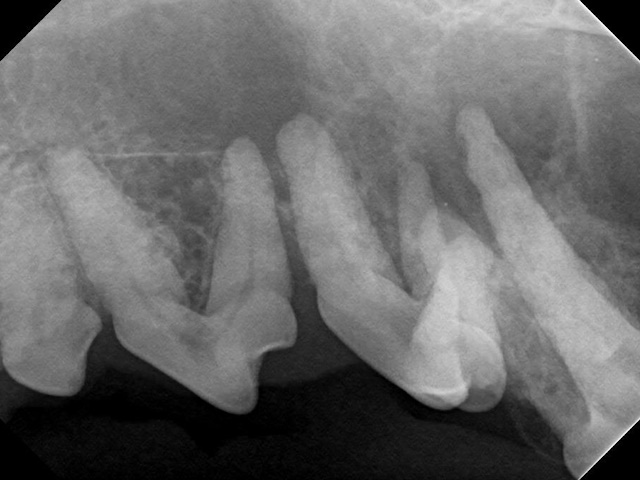
Intraoral radiograph shows significant bone damage around the roots of the premolars.
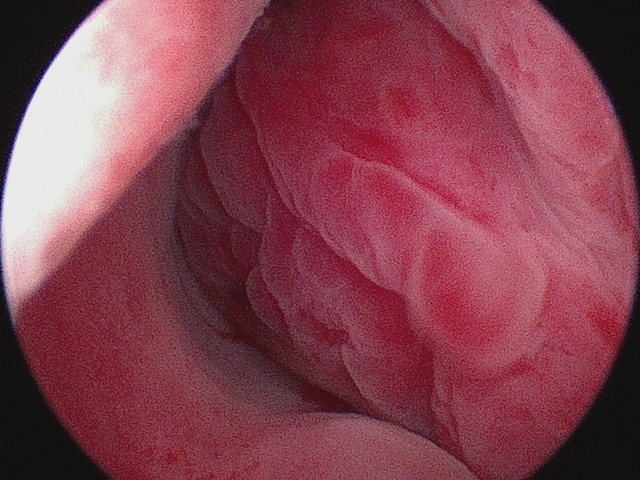
Rhinoscopic (endoscopic) examination of the left nasal cavity showed a soft tissue mass. Both the intraoral and the intranasal masses were diagnosed as osteosarcoma with biopsy.
Peripheral Odontogenic Fibroma
Peripheral odontogenic fibroma (POF) is the most common benign oral tumor in dogs, originating from the cells of the periodontal ligament. While benign and non-metastatic, POFs are considered locally aggressive because they grow continuously and can eventually displace teeth or invade adjacent oral tissues if left untreated. The calcified version (previously known as an ossifying epulis) contains varying amounts of bone-like material, which makes the mass firmer and often more challenging to excise compared to the purely fibrous type. Treatment requires complete surgical excision, typically performed through an en bloc resection that includes removing the mass, the associated tooth, and performing curettage of the tooth socket to eliminate any remaining ligament cells. The prognosis is excellent, with a cure rate of approximately 95% following successful removal with clean margins. Recurrence is rare (estimated at less than 5%) when proper surgical techniques are used, though incomplete excision increases the risk of mass regrowing.
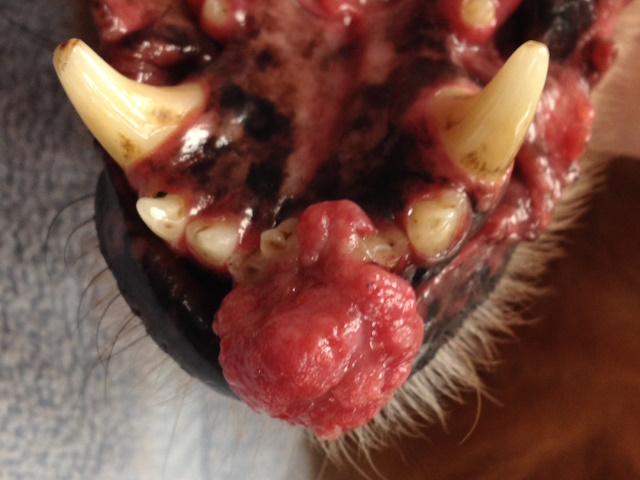
A large, proliferative mass around the lower incisors, biopsy showed it was a peripheral odontogenic fibroma.
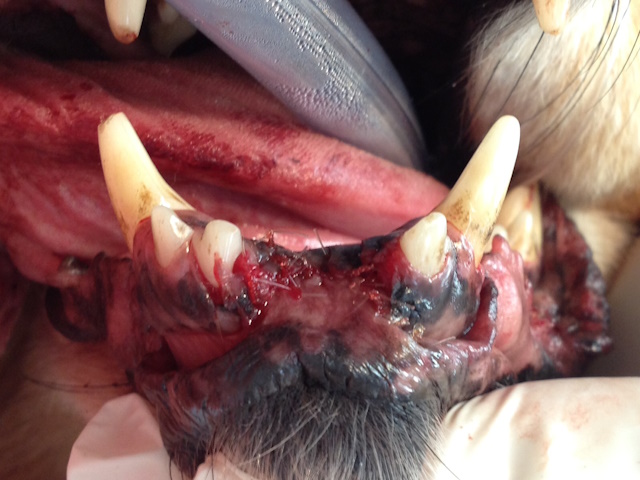
Narrow margin excision with extraction of nearby incisors and complete curettage of their sockets was performed to prevent recurrence.
Prognosis in Cats
Squamous Cell Carcinoma
Feline oral squamous cell carcinoma is the most common oral tumor in cats, typically carrying a guarded to poor prognosis because most cases are clinically advanced and highly invasive at the time of diagnosis. While a cure is potentially possible for a small subset of cats whose tumors allow for wide surgical margins—or resection followed by definitive radiation therapy—most cases are non-resectable and prone to local recurrence. For these advanced tumors, even aggressive treatment combining high-dose radiation and chemotherapy generally results in survival times of less than six months. Consequently, treatment is primarily aimed at palliation to improve quality of life, as standard interventions have a limited impact on overall survival.
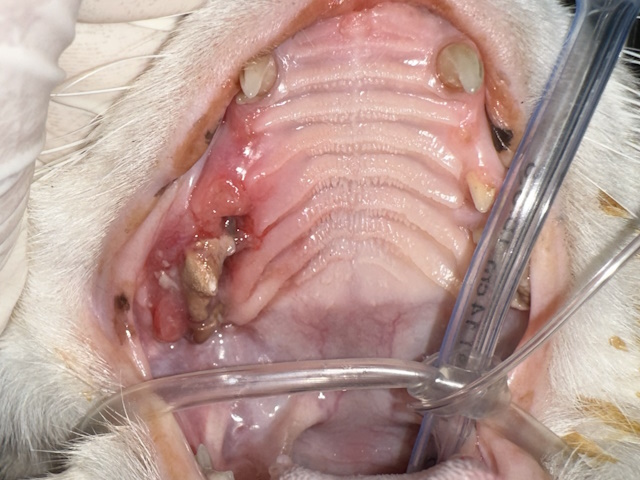
Severely inflamed gums and oral mucosa affecting the third and fourth premolar area. Deep biopsy of this region revealed squamous cell carcinoma.
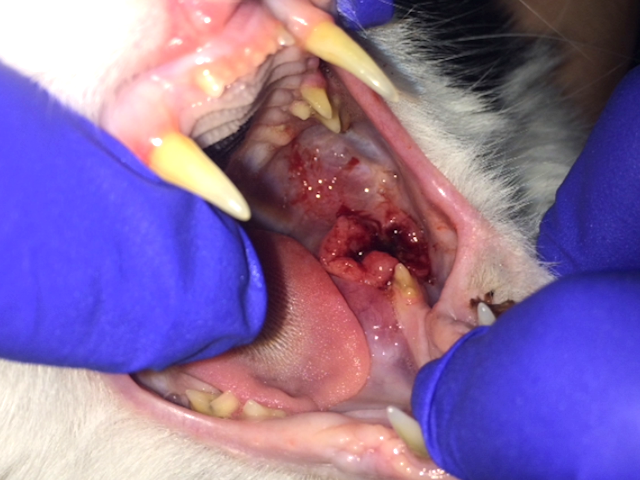
Hyperplastic, ulcerative and bleeding lesion in the caudal mucosa and mandible. Biopsy showed squamous cell carcinoma.
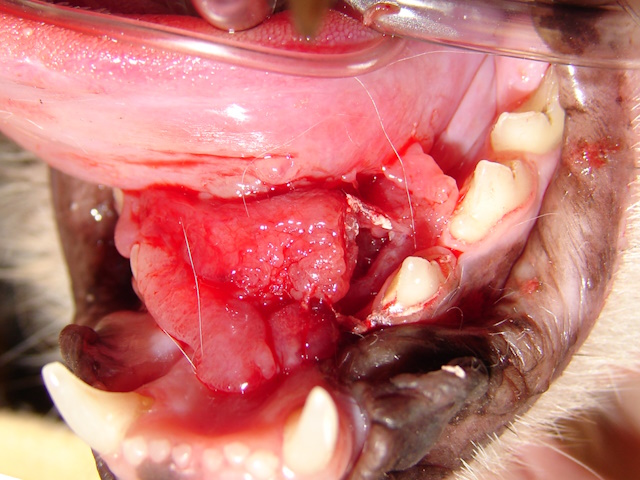
Ulcerative and bleeding growth under the tongue. Biopsy revealed a sublingual squamous cell carcinoma.
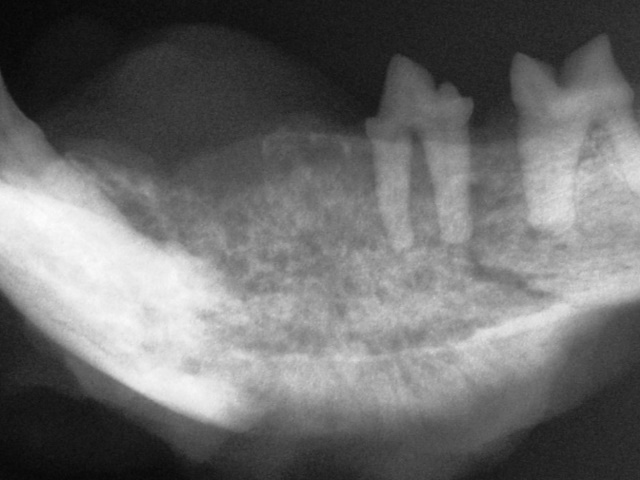
The mandible of a cat shows severe, diffuse, poorly marginated bone destruction with loss of normal bone architecture consistent with an aggressive process. Biopsy showed squamous cell carcinoma.
Fibrosarcoma and Osteosarcoma
Feline fibrosarcoma and mandibular osteosarcoma appear to have more favorable outcomes than feline SCC when complete surgical excision is achieved. Cats undergoing mandibulectomy for osteosarcoma may experience long-term survival with low recurrence and metastatic rates.
Conclusion
In conclusion, oral tumors in dogs and cats require a thorough diagnostic approach and careful treatment planning. Surgical excision remains the foundation of therapy, with adjunctive modalities improving outcomes in selected cases. Early detection, accurate staging, and appropriate tumor-specific therapy are critical for maximizing survival while maintaining acceptable quality of life.
